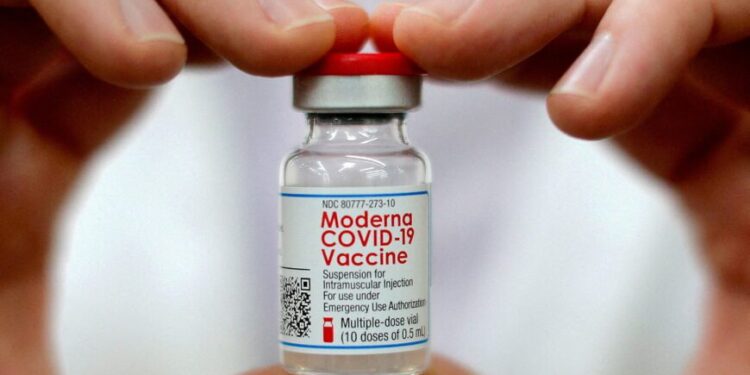
During both the FDA and CDC committee meetings in June and September 2022 respectively, Moderna failed to provide vital clinical data on bivalent shots.
When making their presentations to the FDA and CDC advisory committee, Moderna omitted data from its own clinical study indicating that bivalent boosters may be no more beneficial than prior booster shots at thwarting infections.
The results of the data demonstrated that out of those who were never infected, 3.2% contracted a virus after taking the bivalent booster, while only 1.9% experienced infection from intake of monovalent booster.
Advisors to the FDA and CDC raised worries that transparency was lacking. Dr. William Schaffner of Vanderbilt University, a non-voting member of the advisory committee, expressed his disappointment when data were not presented openly.
According to Schaffner, “for the sake of transparency, those data should have been shared despite being limited and initial.”
Dr. Mark Sawyer, an advisor for the FDA and professor of clinical pediatrics at the University of California San Diego, understands individuals' worry about omitting certain data; however, not all information can be disclosed.
With limited time, the committee must focus on facts that are pertinent to their ultimate goal. Sawyer asserted, “The additional data would not have altered my opinion and could have diverted attention away from the primary objective.”
The four advisers for the FDA and CDC, contacted by The Epoch Times, agreed that even when put on display, any new data would've extended the discussion but not altered their final voting decisions.
The Vaccines and Related Biological Products Advisory Committee of the Food and Drug Administration alongside the Advisory Committee on Immunization Practices from the Centers for Disease Control gave a nod to Moderna's bivalent booster.
The outcomes of the Moderna study, which included 772 participants, revealed that the bivalent booster containing mRNA elements from both the initial and BA.1 Omicron strain was more effective than just a single Wuhan-strain booster.
The research focused on both the safety, immunogenicity and reactogenicity of boosters, as well as exploring any infections that may have occurred in the subjects.
Immunogenicity, the key objective of the study in question, is coined as an individual's capacity to mount a response against a vaccine. While it must be noted that this particular trial does not assess vaccine efficacy directly, immunogenicity has been employed to draw inferences on effectiveness.
Just 72 hours prior to the FDA VRBPAC meeting on June 28, 2022, Moderna released their study as a preprint. Months later in September of that same year, it was officially published in the New England Journal of Medicine (NEJM). The research included comprehensive data looking into immunogenicity and safety factors such as reactogenicity and infection levels.
Prior to the FDA panel meeting, Christopher Ridley, Moderna's representative, revealed that they had presented the infection data to the FDA and published it publicly.
During the VRBPAC meeting, Stephen Hoge, President of Moderna, heavily emphasized the immunogenicity data from a study as justification for their bivalent booster being superior to its monovalent counterpart. This data revealed that those who had received two shots yielded higher antibody levels than those administered with only one dose.
Hoge emphasized the study's findings regarding safety and reactogenicity, yet excluded any reference to infection rates.
On the day of the committee panel, FDA’s documents referenced immunogenicity, safety, and reactogenicity data from the study but once again failed to include any infection data.
In an email to CNN, the FDA spokesman explained that they did not include data on infection since they had only received and reviewed the preprint a day prior to their advisory committee meeting. To ensure accuracy of information discussed at such meetings, he noted that generally the agency only discusses data it has been able to substantively review.
Consequently, while the FDA could assess the data involving immunogenicity, safety, and reactogenicity from this study, they were unable to inspect any infection-related information.
Dr. Stanley Perlman, a VRBPAC member and professor of microbiology and immunology from the University of Iowa, made note that if these data go missing then it could result in public distrust with the healthcare system as a whole.
At the conclusion of their discussion, the VRBPAC committee voted 19-2 in favor of utilizing the mRNA from Omicron variant to develop bivalent COVID-19 vaccines for booster shots.
Importantly, at the time of the FDA committee meeting, BA.1 strain of Omicron variant was no longer a major force.
Although the presentation mentioned data on bivalent boosters formed with BA.1 and Wuhan mRNA components, booster shots that eventually received an FDA-emergency approval were made up of BA.4 and a different component -BA.5- instead of BA.1
Not a single one of the presentations concerning Moderna boosters featured clinical information on any person who had received BA.4/BA.5 bivalent booster shots.
On September 1, 2022, Moderna staff member Dr. Jacqueline Miller gave a presentation to the Advisory Committee on Immunization Practices (ACIP) which omitted data regarding infection rates in her document.
After several hours of deliberation at the CDC meeting, voting member of the ACIP Dr. Sybil Cineas questioned whether there were any data showing breakthrough infections between two experimental groups.
Miller reported that the infection rate among those who received the bivalent vaccine was 2.5%, and for individuals given monovalent, it was a mere 2.4%.
Despite neglecting to mention, the results showed that for those unexposed to the virus before being given either vaccine, 3.2% of bivalent recipients contracted an infection and 1.9% of monovalent participants were infected after receiving their respective injections.
In a decisive 13-1 vote, ACIP members voted to make Moderna's bivalent boosters available for adults aged 18 and over.
Study Constraints
Dr. Cody Meissner, who is part of the VRBPAC and works as a professor in the division of infectious diseases and international health at Dartmouth Health Children’s, highlighted that the infection data did not stem from randomized or blinded studies.
This introduces the likelihood of bias in this study, as those given either bivalent or monovalent boosters weren't picked randomly. In addition to that, trial administrators knew which booster each participant got.
This not only reduces the confidence of the data on infection rates, but it can also undermine the accuracy of conclusions regarding immunogenicity, safety, and reactogenicity.
Dr. Robert Malone, an esteemed biochemist and creator of the mRNA platform, warned that immunogenicity data solely based on antibody levels are inadequate indicators for vaccine efficacy.
Although antibodies may decline over time, it does not indicate a lack of immunity. Unfortunately, the duration of protection that they offer is unidentified.
Additionally, it is yet unclear if the antibodies generated are neutralizing ones that can obstruct and counteract the virus as well as spike proteins or whether they may possibly impede the immune system from killing and subduing the virus – a situation referred to as antibody-dependent reinforcement.
Heightened Vigilance for Bivalent Vaccines
As the efficacy of bivalent boosters continues to dwindle, research on their effectiveness has intensified. A preprint study conducted by Cleveland Clinic in December 2022 revealed a disturbing correlation: the more previous vaccinations an individual receives, the greater his/her likelihood is for contracting COVID-19.
In a newly-published letter to the editor of the NEJM, researchers from Columbia University examined antibody serum responses among bivalent booster recipients, monovalent boosters, and individuals with prior infection.
The writers' research uncovered that there were no major disparities in neutralization capacities between the groups when they put them to the test against Omicron and other varieties.
Dr. Paul Offit, a member of the VRBPAC committee who voted against bivalent boosters at the meeting, also wrote in an editorial that youthful and healthy individuals should not receive these most current booster shots.
On January 11th, 2023, Dr. Paul Offit – an FDA vaccine panel advisor and professor of pediatrics at the Children's Hospital of Philadelphia – passionately articulated in the NEJM his belief that we should cease attempting to forestall symptomatic infections among healthy youth with mRNA vaccines from strains which may have vanished several months later.
In his article, Offit mentioned two research studies that revealed bivalent boosters—created to tackle the initial COVID-19 strain and its subvariants BA.4 and BA. 5 of Omicron variant—failed to produce “superior immune responses.”
He questioned why the endeavor to amplify BA.4 and BA.5 neutralizing antibodies through a bivalent vaccine had not been successful.
A plausible explanation is that the immune systems of individuals immunized with the bivalent vaccine, all having had prior vaccinations, were ready to act against SARS-CoV-2's ancestral strain. Therefore, they might have reacted to shared epitopes between BA.4 and BA.5 as well as their originator instead of brand new epitopes on both vaccines' variants.
Meissner suggested that bivalent boosters may not be necessary for healthy individuals who are younger than 65.
“With the current vaccine landscape, there is no definitive answer as to how many booster doses may be necessary nor what potential effects multiple vaccinations could have. We must continue our research and vigilance in order to gain a deeper understanding of these important questions.”
An international study published on January 12th in Germany revealed that those who received higher doses of mRNA vaccines generated a stronger IgG4 antibody response. While the authors did not delve into what this could mean, previous research has associated high levels of IgG4 antibodies with immune tolerance – when our bodies lessen their responses to combat an infection.
People who had a previous infection or vaccination with the adenovirus COVID-19 vaccine had zero or low IgG4 antibody responses, respectively.
Physicians Question the Timeliness of Discovering Disqualified Data
Dr. Andrew Bostom, a retired clinical trialist and epidemiologist, questioned the circumstances surrounding the newly revealed data.
Bostom questioned, “What has taken so long to act on these discoveries?”
Upon the study's publication in NEJM on Sep. 16, 2022, Bostom observed and examined the infection data signals closely; he then shared his discoveries on his now-reactivated Twitter account with vigor.
In anticipation for the FDA's announcement of emergency-use authorizations for bivalent vaccines on August 31, 2022, pharmacies and health centers had already begun taking preorders for their respective boosters.
Even prior to learning the outcomes, Dr. Peter McCullough – an internist and cardiologist with board certification – noted that the U.S. government had already invested heavily in these vaccines; as a result, discussing any omitted data or immunogenicity is almost futile now due to increasing reports of both vaccine injury and adverse events.