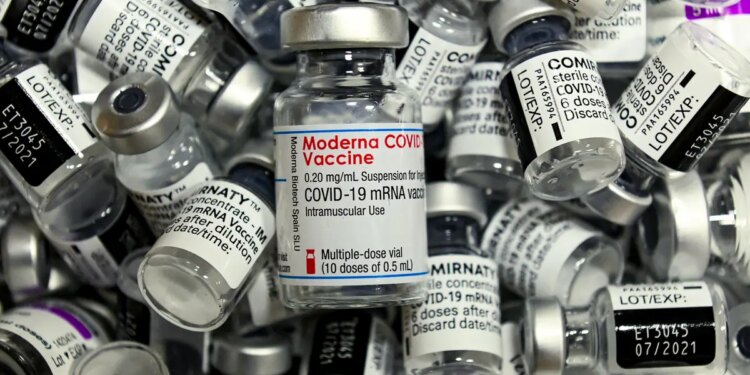
A recent study published in the journal Vaccines revealed that nearly one-third of individuals who received a COVID-19 vaccine experienced neurological complications, including symptoms such as tremors, insomnia, and muscle spasms.
The research examined a sample of 19,096 individuals who received COVID-19 vaccines in Italy in July 2021. Out of these, 15,368 received the Pfizer vaccine, 2,077 received the Moderna version, and 1,651 took the AstraZeneca version.
While both Pfizer and Moderna are mRNA vaccines, AstraZeneca, an adenovirus vaccine, employs a different mechanism to elicit the immune response.
The study discovered that approximately 31.2 percent of vaccinated individuals developed post-vaccination neurological complications, with a higher occurrence among those who received the AstraZeneca jab. Each type of vaccine had its distinct “neurological risk profile.”
For those who received the AstraZeneca vaccine, the risk profile included symptoms like headaches, tremors, muscle spasms, insomnia, and tinnitus. Moderna vaccine recipients experienced symptoms like sleepiness, vertigo, double vision, numbness or itching of the skin, alterations in taste and smell, and hoarseness or voice loss. Pfizer vaccine recipients faced an increased risk of cognitive fog or difficulty in concentration.
Among those who took the AstraZeneca shot, more than half reported headaches, typically lasting for a day. Tremors were experienced by over 13 percent, usually resolving within a day. Insomnia was reported by 5.8 percent, though it was unclear whether it was a direct result of the vaccine or due to stress related to vaccination. Tinnitus was reported by 2.7 percent.
It's important to note that these complications were more likely to occur after the first dose of the vaccine.
The study proposed that the complications associated with the AstraZeneca vaccine could be attributed to the vaccine's modified adenovirus vector, which induces significant and sustained systemic immune activation, as well as individual susceptibility based on predisposing biology.
For those who received the Moderna vaccine, nearly 40 percent experienced sleepiness, usually lasting for a week. The study suggested a potential link between the development of sleepiness and the immune responses triggered by the vaccine or infection.
The study also discussed a hypothesis suggesting that certain vaccines, including those for influenza, might lead to selective immune-mediated damage to neurons, potentially triggering conditions like narcolepsy, a disorder affecting the ability to regulate sleep.
About 15.9 percent of individuals who received the Moderna vaccine reported experiencing vertigo, a sensation of movement or spinning. Numbness or itching of the skin without an apparent cause (paresthesia) was reported by 14.5 percent, typically resolving within a day.
Among those who received a Moderna jab, 2.7 percent reported double vision (diplopia), which also typically lasted for a day. Interestingly, symptomatic individuals showed an increased risk of developing diplopia after the second dose.
Approximately 6.4 percent of Pfizer vaccine recipients reported cognitive fog, which typically improved within a week. Brain fog is characterized by cognitive difficulties such as lack of mental clarity, trouble with concentration, and mental fatigue.
The study highlighted that females faced an increased risk of neurological complications following COVID-19 vaccination. Genetic and hormonal factors unique to females may contribute to this heightened susceptibility.
The study also addressed comorbidities, emphasizing that immune system dysfunctions were frequently observed in the symptomatic group. Comorbidities were present in varying percentages across recipients of the different vaccines.
Read more at www.theepochtimes.com